 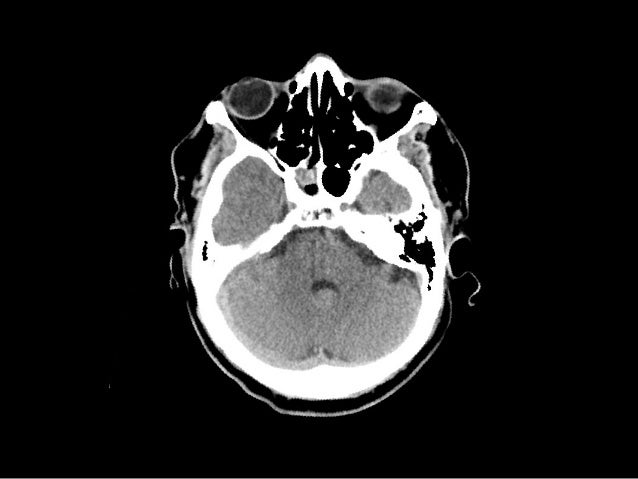
1, 2 Potential pathogeneses include cardiac emboli, large-vessel atherosclerosis, vertebral artery dissection, local arterial disease, and less commonly hypercoagulable conditions, vasculitis, venous sinus thrombosis, and drug use. This case demonstrates several important points about cerebellar infarcts including the disproportionate number of posterior circulation strokes after cardiac catheterization, the difficulty recognizing cerebellar infarctions and, most importantly, the potential for rapid deterioration requiring urgent neurosurgical intervention.Ĭerebellar infarcts are relatively uncommon and represent ≈2% of all ischemic strokes. C, Within 48 hours, cerebral edema effaced the fourth ventricle, enlarged the temporal horns of the lateral ventricles, and compressed the brain stem. B, Infarcts were clearly evident on MRI at 6 hours. A, Initial computed tomography head showed questionable cerebellar infarcts at 5 hours of symptoms. At the time of discharge, she had severe bilateral upper extremity dysmetria and was nonambulatory.įigure. After surgery, her mental status improved. Forty-eight hours after the catheterization, she became obtunded, and CT of the head showed worsening posterior fossa edema and obstructive hydrocephalous ( Figure), requiring placement of an external ventricular drain (EVD) followed by urgent suboccipital decompressive. The next morning aspirin and clopidogrel were held in favor of heparin, in case she required neurosurgical intervention. She was started on low-dose aspirin and clopidogrel and transferred to the Neurological Intensive Care Unit for monitoring. Emergent noncontrasted computed tomography (CT) of the head showed questionable bilateral cerebellar infarcts that MRI confirmed ( Figure). Her examination was significant for lethargy, dysarthria, bilateral upper extremity ataxia, and bilateral inferomedial gaze deviation. 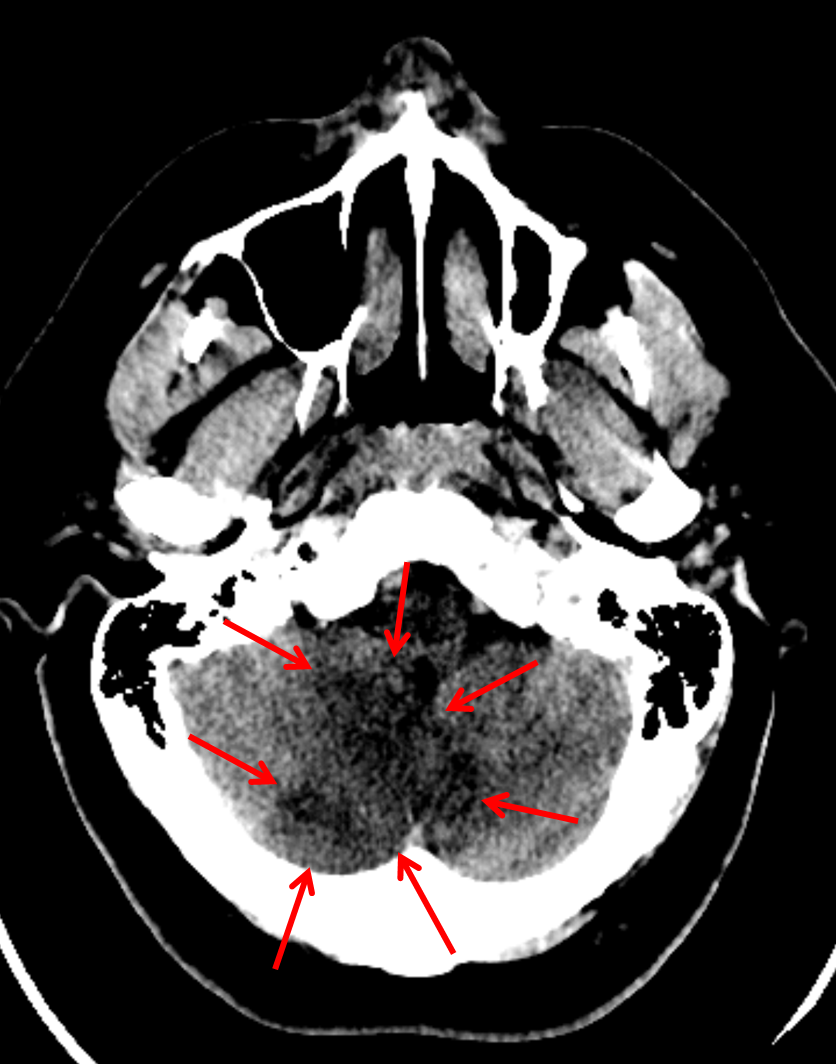
She was nauseated with continued vomiting. Initially, the patient’s systolic blood pressure was >180 mm Hg. Initially, her symptoms were attributed to sedation however, after failing to improve four hours later despite treatment with opioid antagonists, urgent neurological consultation was obtained. Customer Service and Ordering InformationĪn 80-year-old woman was admitted for lethargy and vomiting after diagnostic cardiac catheterization.Stroke: Vascular and Interventional Neurology.Journal of the American Heart Association (JAHA).Circ: Cardiovascular Quality & Outcomes.Arteriosclerosis, Thrombosis, and Vascular Biology (ATVB). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
